Humans are omnivores but does that mean we need to eat plants AND animals?
To address this, we first need to ask 2 questions:
1) need for what?
2) need vs. optimization?
STORY TIME
Scientists were determining the amino acid requirements of cats by feeding them semi-synthetic diets with various levels of each amino acid, one at a time. Tedious. A lot of cats x a lot of amino acids x a lot of levels of each amino acid = a lot of work. What made it even more difficult (and equally more interesting) was that they didn’t know what they were looking for — this was long before we knew what we know now about biology.
Tyrosine
Funny thing, when they got to tyrosine: below a certain level and their black cats started turning red! At an even lower level, certain neuroloogical abnormalities set in. So, how much tyrosine do cats need? Enough to maintain their beautiful black coats? I think we can all agree that the level which induced neurological abnormalities was too low. What about fur color?
What if female cats prefer males with beautiful black coats? So the males have a better chance at reproducing if their diet is at the higher level of tyrosine. I’d say fur color is pretty important in this #context! [how ya like ‘dem apples]
Need vs. Optimization
Note: this occurred over the course of weeks-to-months, not hours-to-days.
Note (2): unlike humans, cats are obligate carnivores. Real, actual, carnivores.
Arginine
Below a certain level of arginine and the cats looked dizzy, wobbled around, and some of them died.
Not weeks-to-months. Hours-to-days. This is what it’s like to be a carnivore. They NEED to eat meat or die rapidly (this is one of the few examples of an acute nutritional deficiency causing severe toxicity in the entire animal kingdom).
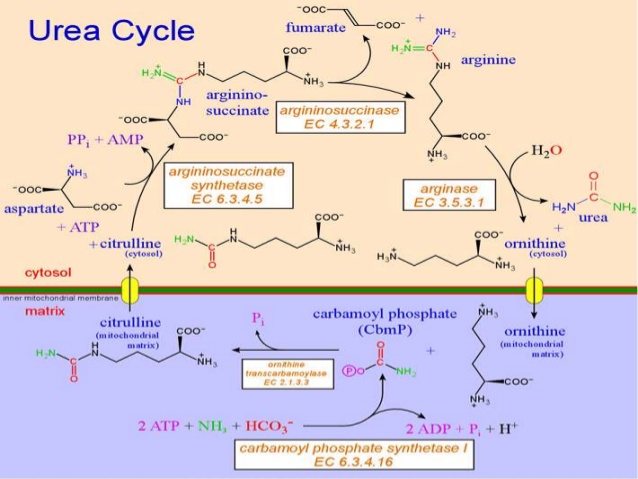
Cats have an inability to downregulate protein degradation and need arginine to dispose of the nitrogens via urea cycle. Humans just reduce burning proteins when protein intake is low.
Part 2. Lobsters are omnivores and arginine is weird.
Lobster tail is rich in arginine (this might be what gives it a bit of a sweet-like flavor). If lobsters are fed an arginine-deficient diet, they go cannibal and eat other lobsters’ tails!
What does this say about lobster arginine requirements?
Need vs. optimization: they’re perfectly healthy, but is preventing cannibalism a “need?”
. . . . . . . .
So, I ask again: Humans are omnivores but does that mean we need to eat plants and animals?
One retrospective study showed stroke victims who had consumed blueberries the day before showed significantly less cognitive decline post-stroke than those who hadn’t. Blueberries. Not green tea, blackberries, or dark chocolate. Blueberries. Do humans need to eat blueberries?
What if this was confirmed in a double-blind RCT? Is preventing post-stroke cognitive decline a need or an optimization?
Which is more important to you?
I didn’t have it in me to put this behind a paywall because while I think the answer is getting simpler & simpler (eg, Sunlight, Hunger-Free Diet[s] and DietFits, hot Blue-Blockers, etc.), fad diets are getting weirder & weirder. Just eat like an adult.
That’s all for now!
For personalized health consulting services -> drlagakos@gmail.com
Check out my Patreon campaign! Full access for a five bucks a month and there are many other options. It’s ad-free and you can cancel if it sucks 🙂
Affiliate links: Still looking for a pair of hot blue blockers? TrueDark & Spectra479 are offering 15% off with the coupon code LAGAKOS. If you have no idea what I’m talking about, read this then this.